Principal Traci Horton, from Burlington’s Grove Park Elementary School, used to work in a school that only had a half-time school nurse.
Never again.
“When I came to Grove Park, I could definitely tell the difference in what my teachers are able to do,” Horton said. “Our teachers have more of an opportunity to instruct which is what they’re supposed to be doing.”
But Horton is in an unusual position for North Carolina. The majority of schools in the state – 58 percent – do not have a full-time health professional on campus.
As a matter of fact, 60 percent of schools in the state do not meet the old recommended standard of one school nurse for every 750 students, which the General Assembly adopted as a goal for North Carolina back in 2004. After a decade of little or no growth in state dollars allocated to the school nurse workforce, a recent legislative report concluded “the General Assembly should direct the State Board of Education to formulate a new goal for school nurse staffing levels and a strategic plan to meet those levels.”
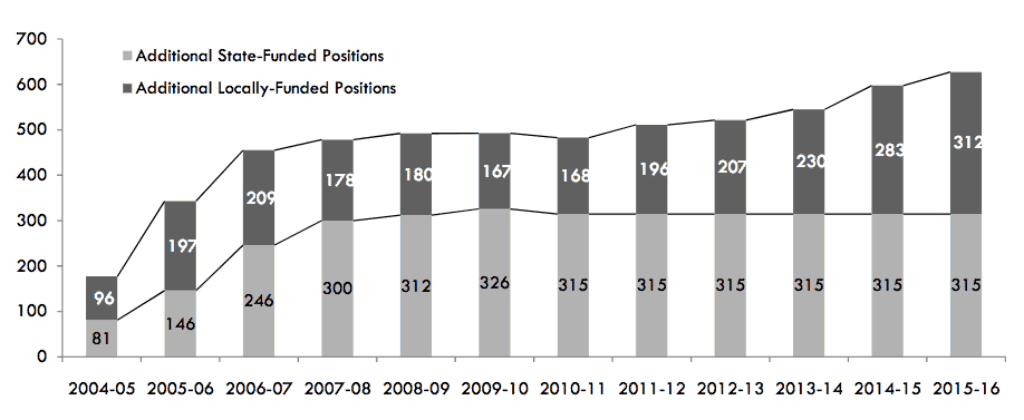
But what the report left unanswered is the question: What is the right number of school nurses for North Carolina?
It turns out the thinking around that has changed since 2004.
Numbers game
The report, penned by the legislature’s nonpartisan Program Evaluation Division after months of study, has yet to be formally presented to or voted on by the Joint Legislative Program Evaluation Oversight Committee, the body that would make recommendations about whether and how to fund the plan. Committee co-chair Rep. Craig Horn (R-Weddington) said he could not comment on the findings until after committee discussion. He did note his ”a record of supporting school nurses in every school in North Carolina and recognizing its importance.”
The report found that instead of there being one nurse for every 750 students across North Carolina, there is only one nurse for every 1,086 students, and to reach the 1-to-750 goal would require about $45 million in state funding.
Credit: Lindsay Carbonell/EducationNC
Legislative analysts also found that 60 percent of medical tasks and three-quarters of medications given to students are done by unlicensed assistive personnel, something that Grove Park principal Horton said can be a distraction for teachers and staff.
“When [the nurse is] out of the building, we are all running around trying to do the job of two people,” Horton said, describing situations where a teacher – or even she – is trying to determine whether a child who feels queasy needs to go home or just needs to lie down for a few minutes.
“We’ve got to determine is it something they ate or is it a virus,” she said. Having a full-time nurse means that “she can meet the needs of our students health-wise so our teachers can meet the needs of our students academically.”
And the legislative analysts found to meet the higher goal of having a nurse in every school would take more: 1,143 more nurses and as much as $79 million in funding.
But those might not be the right numbers either.
Acuity model
The 1-to-750 number is an old goal, and the National Association of School Nurses no longer endorses it. Instead, the group is advocating for a more nuanced approach, said Donna Mazyck, who heads the organization. She admitted the 1-to-750 goal did not have a lot of hard evidence behind it when they first promoted it 20 years ago. Since then, there has been research around finding a way to determine how much school nurse time a school needs.
Using an acuity model to assign nursing staff is old hat in health care; hospitals use them all the time to determine the staffing for a unit on a given day by looking at the needs of the patients in the beds.
There has been less effort on creating school nurse acuity models, however. Some of the latest research on the issue comes out of Wake County, where nurse Donna Daughtry from Wake County Human Services, along with the Kelly Creech, who directs health services for the school district, worked to create such a model.
“We knew that the nurse to student ratios, the 1-to-750 that was recommended by NASN, was not really working for us,” Daughtry said. “We just began to have conversations about how we could do it differently and how we could gather our data.”
Working with Martha Engelke, a nurse researcher based at East Carolina University, Daughtry and Creech created a model that gives weight to schools based on certain criteria: the bulk of the weighting in the model was given to so-called “social determinants of health” factors that fall outside of the provision of hands-on care. These determinants are increasingly being recognized for their influence in whether a person is healthy and can stay that way.
For Daughtry, Creech and Engelke, the two largest factors included the state’s school report card performance score and the number of children at the school who receive free or reduced meals which measures school quality. Research has repeatedly shown that kids from such low-income families had more demand for nursing services, in part because these kids tend to have more chronic health problems, from asthma to diabetes to learning disorders.
“Only 20 percent of the formula was allotted for identified health conditions and medical procedures,” notes Daughtry’s and Engelke’s study, which was published in the Journal of School Nursing last year.
Over the course of three years, Daughtry and Creech tweaked the way they weighted schools in order to determine the allocation of school nurses across the county, collecting data along the way. Meanwhile, Wake County commissioners stepped in, funding a total of 39 additional nurses over the course of the study period.
“The county really wanted us to look at really proving that the acuity model worked,” Daughtry said. “We’ve revamped it. We recalculated for schools based on the percentage weight in the acuity model, and then we tweaked the amount of nursing hours… as we increased the numbers of hours at a particular school.”
Over the time of the study, many schools have gotten one additional day per week of having a nurse on campus.
Now Wake County schools have 106 nurses overall, with 100 of them paid for by county dollars. And only a handful of schools have a nurse only one day each week.
“The eight-hour schools perhaps have been identified as having kids who are being serviced well in terms of physician care, nursing, those sort of things,” Creech explained. “They are schools that have needs that have been identified and are being addressed.”
Reality bites
All 502 children at Burlington’s Grove Park Elementary qualify for free meals at the school, something principal Traci Horton argued means there is a need for the kind of monitoring that school nurse Amy Widderich provides.
During a recent visit, Widderich showed off a cabinet full of asthma inhalers hung on the wall above drawers full of medications.
“We’ve got kids with diabetes and she has to figure out their plans for care,” Horton said. “We have a student who’s battling cancer and we have a plan for her care. That’s not to mention the broken bones, flu and strep and all the other issues.”
Widderich does more than just take temperatures and screen kids for hearing loss. She helps kids and their families get access to care, something that’s often a challenge for families of low-income worker who often do not get health insurance through a job.
Horton described a recent incident where a child at Grove Park broke their glasses and could not see “at all.”
“Sometimes if you don’t have the insurance, you can’t afford to get glasses until the next year,” she said. “Amy reached out to find the resources to get the student glasses donated so the parent didn’t have to worry about the child being able to see.”
“Sometimes, more often than not, in the school where you have students who are low income, they may not have the means to do all they want to do,” Horton continued. “When you have a nurse full-time there, it’s more of an equalizer. She can advocate for them.”
This story originally appeared in North Carolina Health News and is shared by EdNC through a content-sharing agreement with nonprofit news organizations in North Carolina.
Recommended reading