
From 2008 through 2011, 3,762 physicians graduated from North Carolina residency programs. Five years later, 39 percent of those physicians—or 1,469 of them—still practiced in the state. Of the physicians who remained in practice in North Carolina five years after residency, 108 of them (three percent), practiced in a rural county.
This data, gathered by the Program on Health Workforce Research and Policy at the Sheps Center for Health Services Research, was presented by Sheps Center Director Mark Holmes at the Association for Health Care Journalists workshop earlier this month. The presentation, “Addressing rural health workforce hurdles,” highlighted that there is not a shortage of physicians in North Carolina. There is a distribution problem.
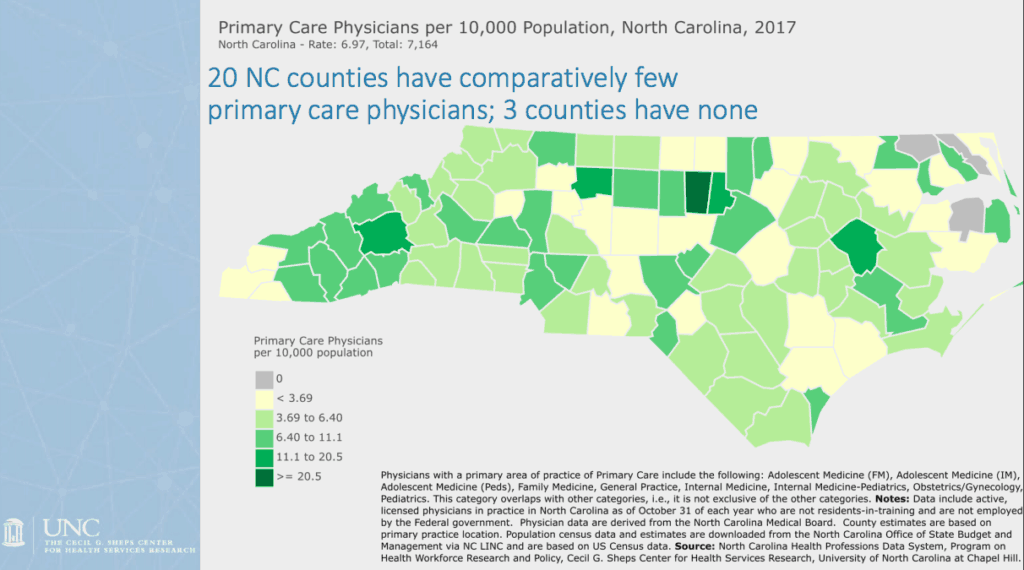
According to Sheps Center data from 2017, there are 20 North Carolina counties that have “comparatively few primary care physicians” and three counties that have none: Gates, Camden, and Tyrrell.
Holmes recognized the challenge of a leaky production pipeline for generating rural doctors — one that starts with recruiting college students from rural and underserved communities to medical school.
“The highest predictor of people who will practice in rural areas is if they’re from rural areas,” Holmes said. However, he said, ideally the pipeline would start well before students were looking at medical school, in elementary school.
“I think certainly as I was growing up in rural Michigan and as a fourth grader [it was], ‘Oh you’re good at math: you should be an engineer,’ and that’s pretty much all we knew,” Holmes said.
Dr. Robert Bashford, associate dean of the Office of Rural Initiatives at the University of North Carolina School of Medicine, co-presented with Holmes at the workshop. Since 2013, Bashford has worked to build the Kenan Primary Care Medical Scholars program, which trains future physicians committed to work in underserved areas, including rural North Carolina.
Kenan Scholars focused on the rural experience undertake a six-week summer internship in a rural practice, serve as mentors for undergraduate and high school students interested in a career in health, and learn about the complexities of rural care through a rural medicine curriculum.
“That’s what we’re basing everything on: that they came from rural settings,” said Bashford of successful Kenan Scholars. “They’ve got to have a rural heart.”
Bashford said he also recognized that rural students did not have the same access to STEM education.
“By virtue of growing up in rural settings, they didn’t have East Chapel Hill High School. They got school in a way that was much different, so they’re not going to score on standardized tests as well,” Bashford said.
“We’ve got to buffer them because we can’t have them flunk out of med school or pharmacy school or social work school, so we’ve got to get them in the pipeline if they haven’t already and help them build an application,” said Bashford.
While North Carolina faces an increasing gap between shortage and non-shortage areas, the state’s economy is also changing. Bashford said while manufacturing jobs are going down, health care jobs are going up.
“There’s a whole workforce going into medicine that can take care of people where they live,” Bashford said.
Recommended reading



