In March 2023, North Carolina gained access to roughly $1.6 billion in federal funds when former Gov. Roy Cooper signed legislation expanding Medicaid. That year, the state budget outlined the state’s plan to spend the funds over the next two years. About half of those funds — $835 million — were directed by the legislature to support behavioral health and resiliency, an unprecedented investment in the state’s behavioral health system.
Over the past two years, the N.C. Department of Health and Human Services (NC DHHS) has overseen most of the $835 million allocation, which includes investments in areas ranging from the state’s juvenile justice system to the state’s behavioral health workforce.
According to a 2024 report that outlined NC DHHS’s planned uses for the funds, and a NC DHHS press release, the largest portion of the $835 million went toward increasing Medicaid reimbursement rates for providers for some behavioral health services. Those rates went into effect Jan. 1, 2024.
Now, updates from NC DHHS are shedding light on how the funds are being used to strengthen behavioral health services across the state.
![]() Sign up for the EdWeekly, a Friday roundup of the most important education news of the week.
Sign up for the EdWeekly, a Friday roundup of the most important education news of the week.
On Feb. 9, NC DHHS released a report detailing the state’s progress on improving its behavioral health system. The report is a one-year update on the Division of Mental Health, Developmental Disabilities, and Substance Use Services’ (DMHDDSUS) 2024-2029 strategic plan and demonstrates the division’s progress on improving mental health services across the state.
As noted in the 2024 report from NC DHHS, the division’s strategic plan was created in part to help advance the behavioral health investment’s roadmap and support sustained attention across its key investment areas. According to the press release, the report highlights key achievements in the strategic plan’s priority areas that were designed to create a “comprehensive mental health care system that works for everyone.”
Separately, an October 2025 presentation from DMHDDSUS Director Kelly Crosbie and two of her NC DHHS colleagues provides a more detailed update on the programs that the $835 million investment has funded.
Thus far, the funds have been used across four categories:
- $120 million for crisis projects,
- $99 million for justice-involved programs,
- $63 million in strengthening the behavioral health workforce, and
- $80 million in child welfare and family well-being programs.
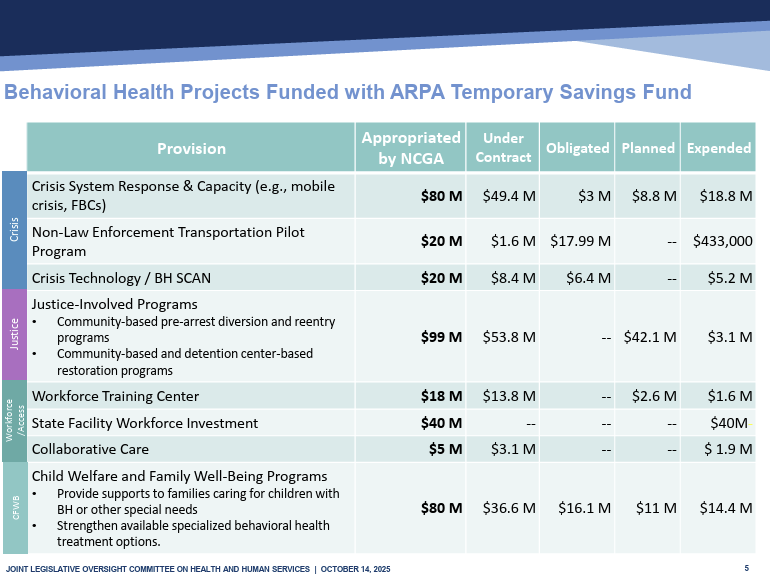
Funds that appear to directly impact school-aged children are those under child welfare and family well-being (CFWB) investments. According to the October 2025 update, CFWB investments were “strategically targeted to improve the health and well-being of youth and family,” with key themes including increasing the availability of evidence-based practices in children’s communities, supporting children in foster care, and investing in specialty residential care.
Four divisions at NC DHHS — DMHDDSUS, Division of Health Services Regulation (DHSR), Department of Social Services (DSS), and the Division for Child and Family Well-being (DCFW) — have collaboratively managed the CFWB funds.
According to the October report, $7 million in investments overseen by the DCFW went toward strengthening behavioral health in schools. In addition to providing school and family support through local health departments across the state, the funds helped to add or expand behavioral health services delivered by existing school-based health centers (SBHC). According to the DCFW, the care provided by the state’s SBHCs provide far-reaching care as they increase adolescents’ access to health care and reduce health and educational disparities.
Funding also went toward expanding access to tele-behavioral health services in rural schools, an initiative that received matching support from The Duke Endowment.
Read more about health in schools


Other investments seek to improve access to behavioral health for youth outside of the school day.
Included under the $99 million in justice-involved investments, for example, the October report highlights Talkspace, a free virtual therapy program available to justice-impacted youth between 13 and 17 years old.
Workforce investments aim to increase the number of behavioral health professionals in the state, as 40% of the state’s population lives in a mental health professional shortage area, per the report.
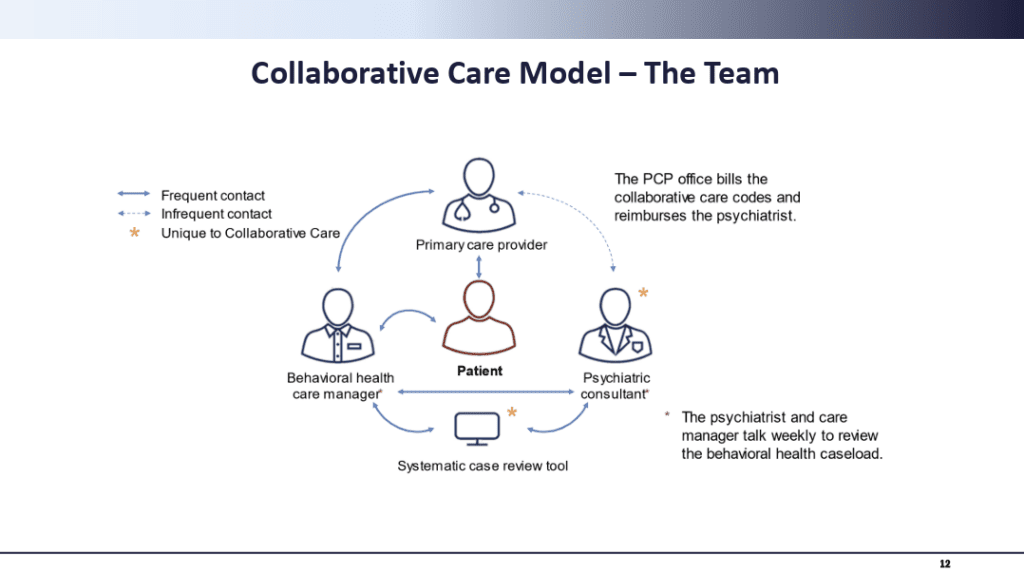
In an effort to close this gap, $5 million went toward expanding the collaborative care model, an evidence-based model that is designed to integrate behavioral health into patients’ primary care settings. As of October 2025, DMHDDSUS has granted scholarships to over 50 practices to aid their integration of the model, in addition to deploying training on the program at the state’s five area health education centers.
Funding has also supported NC-PAL, a psychiatry access line (PAL) for primary care providers whose goal is to improve behavioral health care for North Carolina youth and families through integrated care.
While these investments primarily offer preventative care, $120 million of the appropriated funds are being used to improve the state’s crisis care system. According to the October 2025 report, those investments will help to “ensure timely, effective care for people in crisis, reduce strain on emergency departments, and connect individuals to the long-term support they need.”
Crisis care funding impacting children includes $66.5 million to expand crisis facilities’ capacity, including the addition of 32 child beds at two planned facility-based crisis centers, 13 new 24/7 behavioral health urgent cares — seven of which are open as of October 2025 — and two new transitional residential treatment homes for youth, one of which has also already opened.
Funds will also strengthen crisis system response and technology, including expanding Mobile Outreach, Response, Engagement, and Stabilization (MORES) teams to eight additional counties and adding two additional lines to the state’s operation of the national 988 Suicide & Crisis Lifeline.
The UNC Sheps Center for Health Services Research announced in August 2025 that two research teams are working on statewide evaluations of both the crisis system and programs targeting children and families in partnership with NC DHHS.
According to the October report, stakeholder engagement has been part of the DMHDDSUS’s approach to allocating the legislature’s behavioral health investment. So far, this has included hosting listening sessions, establishing advisory groups on each pillar of the funding, and hosting virtual monthly “Side by Side” update webinars that are open to the public and available to watch on the department’s website.
Editor’s note: The Duke Endowment supports the work of EdNC.
Recommended reading