
When students at Apple Valley Middle School in Hendersonville feel sick during the school day, they don’t have to worry about whether someone can come pick them up to take them to a doctor. Instead, they can just walk down the hall. That’s because Apple Valley is home to one of North Carolina’s oldest school health centers (SHCs), operated by Blue Ridge Health.
SHCs are essentially doctors’ offices located at a school. They can be located in a repurposed classroom space or a standalone structure on the school property. They employ at least one advanced practitioner—a physician, physician assistant and/or nurse practitioner—to see students throughout the school day. The main goal of SHCs is to provide greater access to medical care while minimizing the amount of time students have to be out of a classroom to receive that care.
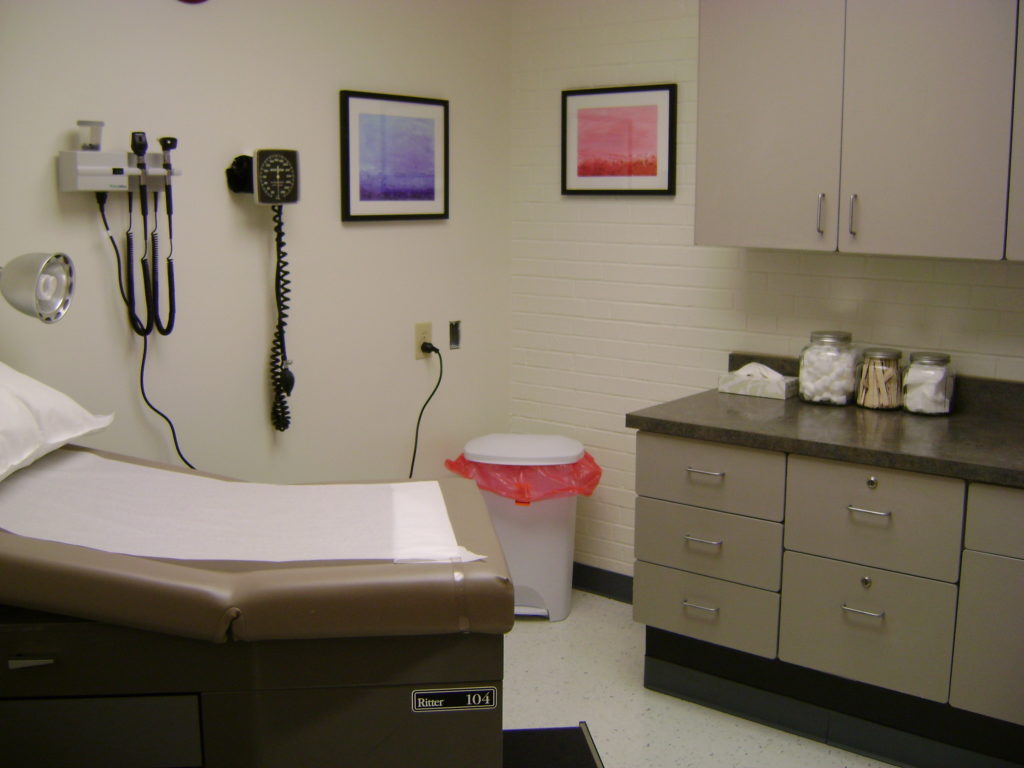
Established in 1996, the SHC at Apple Valley Middle School was the first of Blue Ridge Health’s 13 SHCs across western North Carolina. Tammy Greenwell, Chief Operations Officer of Blue Ridge Health, explains, “We chose a middle school because that’s when health outcomes started falling off. Kids aren’t getting well-child checks anymore. They’re not going to the dentist. Preventative care starts slipping. And of course, there’s mental health issues.” Apple Valley now serves as a model for how traditional SHCs function to improve student access to health services.
When students at schools like Apple Valley feel sick, they can request a medical visit. The student would then leave the classroom to be examined by a physician assistant or family nurse practitioner at the on-site SHC. The clinician would provide appropriate treatment, typically enabling the student to return to class. School staff members can also refer students to the SHC if they notice a child showing symptoms of illness. Without an SHC, students either go without medical care or miss more essential class time by being removed from school for a medical visit off-site.
Ninety-five percent of student guardians at Apple Valley have granted prior authorization for their children to see medical professionals on campus. In a given year, about 700 of the school’s approximately 900 students have used at least one service provided by the SHC.
Starting a full-fledged school health center is no small undertaking. Blue Ridge Health estimates it costs around $30,000 to establish the physical site of an SHC on a school campus. Add in the cost of staffing and the price tag can be daunting. But for existing community health centers or county health departments with access to funding streams, building a SHC provides students, teachers, and families with greater access to health services, potentially improving public health.
Apple Valley Middle School is just one of Blue Ridge Health’s 13 SHCs. To staff its sites, Blue Ridge Health employs four clinicians, six nurses, eight counselors, three medical assistants, a dietician, and a practice manager. Like a traditional doctor’s office, Blue Ridge Health bills patients or insurance companies for visits. It collects about 66% of its revenue through billing, including billing Medicaid.
North Carolina’s Department of Health and Human Services issues grants of $44,400 for qualified school health centers on an annual basis, through a grant proposal process. Blue Ridge Health regularly receives these grants, “which basically cover the cost of one nurse for the year,” says Greenwell. Additional funding comes from federal grants covering uninsured patients, as well as grants and donations from private corporations and charitable foundations.
A major challenge in measuring outcomes for all SHCs, including those operated by Blue Ridge Health, is the inability to merge health data (protected by HIPAA) with educational data (protected by FERPA). This makes it virtually impossible to show whether improved access to medical care has an impact student learning. While academic studies indicate a positive correlation between health and educational outcomes, individual SHCs like the one at Apple Valley Middle School are unable to demonstrate this correlation for themselves.
Blue Ridge Health is in a unique position to collect longitudinal health data for the first time because it recently opened an SHC at Edneyville Elementary School, the feeder school for Apple Valley Middle. Apple Valley is the feeder for North Henderson High School, another Blue Ridge Health SHC site. This will be the first time Blue Ridge Health has the potential to serve students and follow their health from kindergarten through high school graduation.
“I’m very interested in whether we can honestly say – with data – that having a school-based health center makes a difference to that kid throughout their life,” says Greenwell.
The coronavirus pandemic will make that research, and the rest of Blue Ridge Health’s work, more challenging. Blue Ridge Health is authorized to provide – and has access to – COVID-19 testing, but there are still many questions about how to implement that testing at its SHCs.
For example, if students return to classrooms and one presenting symptoms of COVID-19 visits a SHC, CDC guidelines prevent that student from returning to the classroom. The student must be isolated until a guardian can provide transportation home, and riding a bus home is not an option. If the student is kept in the SHC, no other students can be served until that student leaves and the facility is thoroughly cleaned. As Greenwell outlines, “We shut that room down for four hours and we wait, then we go in and clean it.”
Alternatively, SHCs lose a significant portion of their utility in cases of students participating in virtual learning. That’s one reason why Blue Ridge Health is considering mobile health units. Mobile health units are vehicles that are outfitted to serve as doctors’ offices. Some county health departments already use them to provide health services to schools. Blue Ridge Health is considering how these units might help them continue to provide health services to students learning virtually.
In the COVID-19 era, organizations like Blue Ridge Health are turning to telehealth as a scalable way of providing greater access to health services. Blue Ridge Health already has 10 telehealth units, which cost about $2,500 each. The widespread implementation of telehealth during the coronavirus pandemic has increased public familiarity with the technology, likely making people more comfortable with receiving health services remotely. While telehealth cannot deliver all of the services of an on-site SHC, it still significantly expands access to health services when implemented in schools.
Greenwell is optimistic about the potential of telehealth to expand the work of traditional school health centers like the one at Apple Valley Middle School. “When I first came to Blue Ridge Health 10 years ago, it was like, ‘You’ve got to have bricks and mortar! You’ve got to have a physical location!’ and I don’t think that’s the case anymore. It’s great that we have those spaces, but to be honest, you can do telehealth now. The ability to scale-up quickly is there.”
This article is part of a series on innovative approaches to health in schools. Find the rest of the articles here.
Recommended reading



