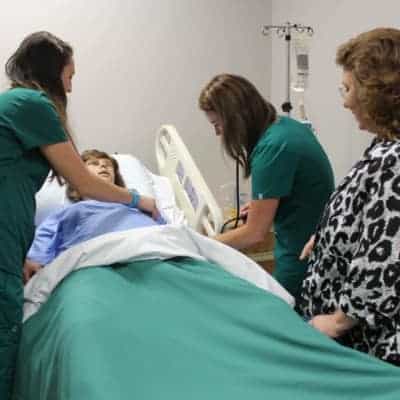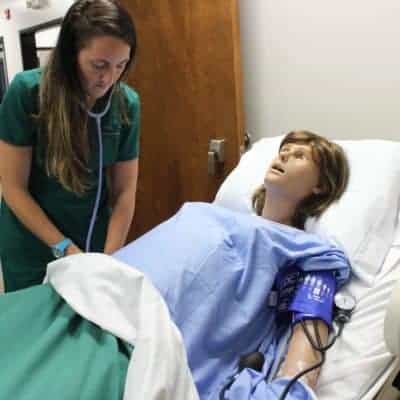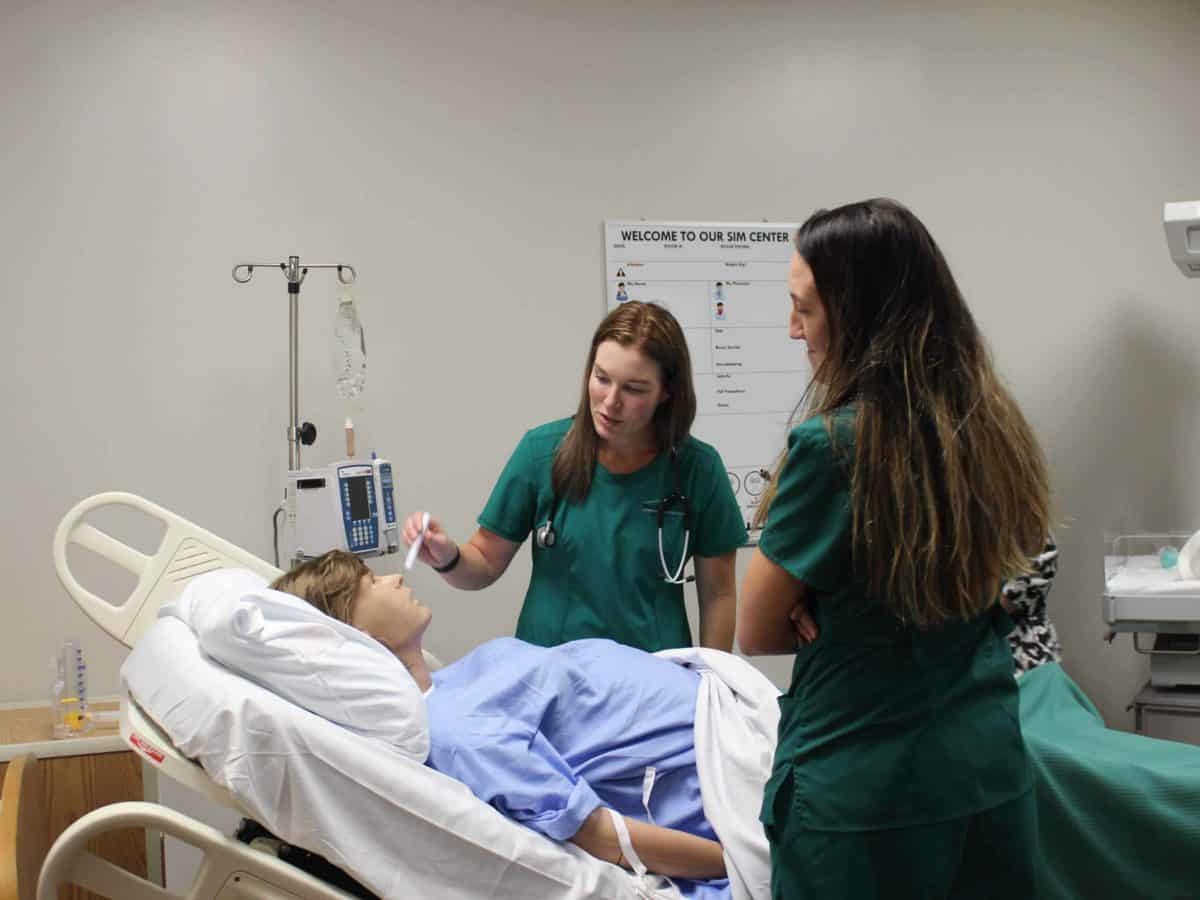
Kara Frogge and Danielle Frizsell, Licensed Practical Nurse (LPN) students at McDowell Technical Community College, stood over their patient. They tested her blood pressure and listened to her heart beat. The patient, Victoria, was pregnant. Gently placing a stethoscope over her belly, they listened to her baby’s faint heart beat, too.
It was their first time meeting Victoria, a $74,000 high-fidelity robot with the ability to simulate birth down to the placenta. Students use Victoria to learn about everything from prenatal, intrapartum, and postpartum care to c-sections and regular delivery, said Judy Melton, dean of health sciences.
Victoria not only simulates a real pregnancy but also a real person—making her invaluable to nurse aide, practical nursing, registered nursing, phlebotomy, and EMS students alike.
“The pupils will constrict and dilate, just like a human,” said Amy Davis, practical nurse instructor, as Frogge and Frizsell shone a flashlight over Victoria’s eyes. And when Frogge moved her finger back and forth over Victoria’s face, the robot’s eyes followed too.
You’ll either find this very creepy or very cool! Meet Victoria. A $74,000 robot who has a heart beat and blood pressure, simulates giving birth, & tracks movement with her eyes. She lives in the @McDowellTechCC sim lab. @EducationNC @NCCommColleges @Awake58NC @mtcc_prez #awake58 pic.twitter.com/FXLuluZDNH
— Yasmin Bendaas (@yasminbendaas) August 27, 2018
“I’m just so thrilled and proud of McDowell Tech that we have the newest cutting edge technology available for our students to have that learning opportunity, to help them prepare for those health care careers out there,” Melton said.
This technology, like Victoria and another high-fidelity robot, Trauma HAL, resides in the Vickie A. Hogan Multidisciplinary Simulation Lab that opened at McDowell Tech in January.
“It gives you a perspective rather than you’re just working on a dummy and it doesn’t do anything, or you just have to act it out. It gives you a real-life interaction,” said Frogge.

In addition to high-fidelity robots, the lab includes several realistic hospital rooms, an indoor simulation ambulance, telemedicine equipment, and a debriefing room. The facility replaces on old electronics lab and was a project ten years in the making.
“If we were going to train our students on state-of-the-art equipment so that they can be ready for the world of work, we’ve got to do whatever we need to do to get that here on this campus, so it was a process,” said Penny Cross, vice president for learning and student services.
The health sciences team had purchased the hospital beds four years beforehand and the large $74,000 purchase of Trauma HAL eight months before the simulation lab’s grand opening.
“Trauma HAL was our first high-fidelity simulator, and he can hemorrhage. He can be a stroke patient. He can be a heart attack patient. You can give him meds intravenously [and] it will actually react as though it was a real person,” said Melton. “Now we can let the student actually make the calls, see what happens based on their calls—was it the right choice to make in that particular instance? Critical thinking’s huge. And then they get to debrief and figure out what they could have done better.”

With Trauma HAL and the indoor moving ambulance, students can also practice taking a patient from a tight space onto a stretcher and safely into an ambulance.
Check out this moving simulation ambulance at the @McDowellTechCC Vickie A. Hogan Multidisciplinary Simulation Lab. The lab just opened in January of this year to prep students to save lives. @EducationNC @Awake58NC @NCCommColleges #awake58 pic.twitter.com/S6hoF9XKUh
— Yasmin Bendaas (@yasminbendaas) August 27, 2018
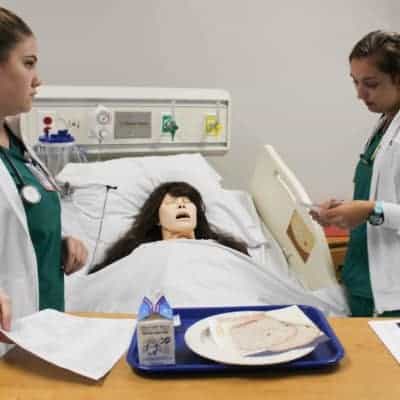
Meanwhile, in the hospital rooms, students work with mid-fidelity mannequins—given hair and eyelashes for a more realistic appearance—to practice dressing wounds, patient interaction, nutrition guidance, and more. Over 100 students have already received hands-on training in the lab and more than 1,000 have toured the facility.
“It’s really perking their interest to look at nursing [and] EMS because they see that we have the cutting-edge technology right here,” said Melton of touring high school students.
However, for Melton, the technology is only a part of nursing training.
“Although I’m a very huge proponent of simulation as a learning technique, nothing can replace actually going in and talking to a real human patient in the hospital,” Melton said. “Nothing can ever replace true hands-on patient care.”
The college extends this philosophy into the treatment of their students, who are often much more than just students. Both Frogge and Frizsell are parents.
Frizsell, who works at Mission Hospital in Asheville as an endoscopy tech, also has a thirteen-year-old son in middle school. “So it’s a little harder working full time and going to school full time,” Frizsell said. “But I have a medical field background.”
Frogge also found the year-long LPN program worth the time and may continue studying to become a registered nurse (RN).
“I have two kids. So this year program, the hours aren’t bad,” Frogge said. “Financial aid helps you a lot. It’s not like you’re going to a university.”
“It’s practical for if you work and have kids.”
Recommended reading