
In-person learning is starting soon amid another coronavirus surge. The StrongSchoolsNC Public Health Toolkit offers guidance on how to return to classrooms as safely as possible.
Find an overview of each safety measure recommended in the guide, which was created by the state Department of Health and Human Services (DHHS) and approved by the State Board of Education this month. Click the links below to jump to each strategy:
First, some context
Unlike last year, students and teachers are heading back for full in-person learning this year. Though the Centers for Disease Control and Prevention (CDC) and Gov. Roy Cooper recommend universal masking, there is no statewide mask mandate and several school boards have voted to make masks optional. Go here to see masking policies for districts across the state.
Vaccines — which are effective against serious outcomes of the coronavirus — are available and recommended for people 12 years and older. Yet vaccination rates vary across the state, and students in elementary schools are not yet eligible for the vaccine.
Go here to see vaccination rates of 12-17-year-olds by county. Go here to see total vaccination rates by county.
The delta variant — now the dominant form of the virus — is much more contagious than the original virus. Without vaccination or prevention strategies like masking, the delta variant spreads from one person to an average of six people compared to the original virus’s spread to an average of two or three people, according to the guide.
“Therefore, unvaccinated people are at greater risk of catching and spreading COVID-19, and they pose a risk to children under 12 who cannot be vaccinated and those who are immunocompromised,” the guide reads.
So what can schools do?
Each section in the toolkit contains two kinds of recommendations: measures schools should take and additional measures schools could take.
“Should” measures, the guide reads, “are strategies that, if not implemented, create conditions of high risk for COVID-19 exposure and spread. NCDHHS strongly advises that school leaders adopt all the strategies in the SHOULD sections.”
“Could” measures “are strategies to provide additional layers of prevention and that, if implemented, will further reduce the risk of COVID-19 exposure and spread.”
Promoting vaccination
Should
Schools should promote vaccination for students older than 12 years old, teachers, staff members, and families. The Pfizer-BioNTech vaccine is available for individuals 12 and older, and the Moderna and Johnson & Johnson vaccines are available for individuals 18 and older.
Schools should take action, the guide says, to support vaccination. This separate DHHS guide provides several options and templates for communication with parents and staff.
Schools should consult with a school nurse, local health department, or health care provider to determine isolation or quarantine when individuals who are only partly immunized are experiencing COVID-19-like symptoms or exposure.
Schools should require teachers and staff to report their vaccination status. The guide says schools should use the same protocols as they use to collect other health information from students and staff, which should comply with “relevant statutory and regulatory requirements, including the Family Educational Rights and Privacy Act (FERPA) and its regulatory requirements.”
Schools should require teachers and staff who are unvaccinated, or do not disclose vaccine status, to participate in screening/testing programs.
Could
Schools can consider hosting on-site vaccination events before, during, and after the school day, during summer months, or during sports or extracurricular events.
Schools can host information sessions about vaccines, boost confidence about vaccination tailored to community needs, or offer vaccination information in kindergarten transition activities.
Schools could offer paid leave for staff and flexible options for excused absences for students to get vaccinated or for potential side effects from vaccination.
Cloth face coverings
Should
The toolkit says all schools should require universal masking for K-12 students and staff regardless of vaccination status when indoors and in group transportation. They should also share information on the proper use of masks and provide masks to students who need them.
When eating, students should maintain at least 3 feet of distance when possible and consider eating outdoors.
If schools do not have universal mask requirements, the toolkit says they should “ensure a layered mitigation strategy, including physical distancing, ventilation, hand hygiene, adequate access to diagnostic and screening testing and closely monitor for increases in COVID-19 cases.”
Physical distancing
Should
Schools should maintain 3 feet of physical distance between unvaccinated students when possible and maintain 6 feet of distance between unvaccinated adults and between students and adults.
For sports teams, there is a separate guide with recommendations and advice for determining risks for different sports.
Could
Additionally, schools can mark floors and seats to remind students to maintain 3 feet of distance and to remind adults to maintain 6 feet of distance. They can also limit staff activities where adults congregate, like during meetings, in teacher lounges, or during breaks.
Schools could allow visitors and parents to resume normal visits to the school if they adhere to the same safety measures as other adults in the building.
Schools could also pick physical education activities that limit opportunities for close contact between students.
Testing
Should
The guide says schools should require screening testing for teachers and staff who are not vaccinated or do not disclose their vaccination status at least once a week — as well as for students if the area’s transmission rate is moderate to high (see table below).
All schools have two options for state-funded diagnostic and screening testing. Schools can decide between a state-contracted testing vendor or independently test students and staff themselves through a vendor not sponsored by the state.
For this school year so far, 144 districts, charter, and private schools have opted into one of the K-12 testing options, according to Catie Armstrong, a DHHS spokesperson. Districts and schools have until Sept. 13 to opt in.
Diagnostic testing is for students or staff who have COVID-19 symptoms or have been in close contact with an infected person. Schools should offer free rapid testing for a quick diagnosis and to determine the necessary next steps.
Screening testing is for students or staff who do not have symptoms or a known close contact. The CDC does not recommend screening testing for fully vaccinated people.
“Screening testing may be most valuable in areas with substantial or high community transmission levels, in areas with low vaccination coverage, and in schools where other prevention strategies are not implemented,” the guide reads. “More frequent screening testing can increase effectiveness, but feasibility of increased testing in schools needs to be considered.”
Schools should create a screening testing strategy based on the following table:
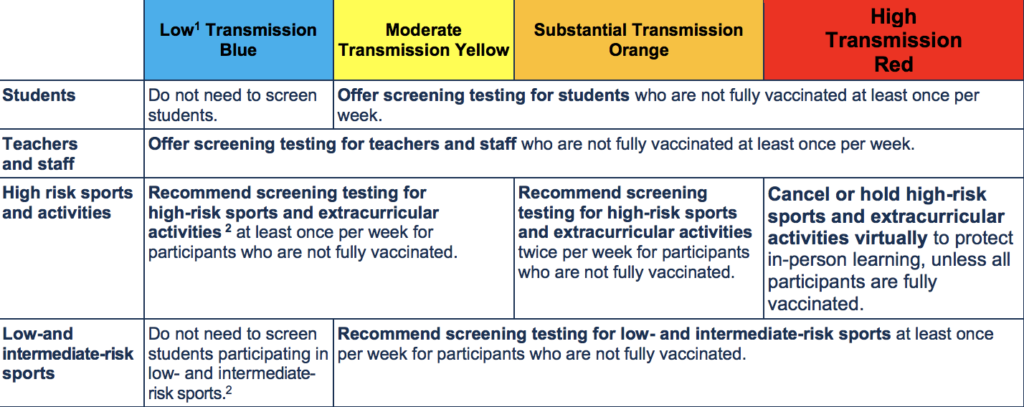
Handling possible, suspected, presumptive, or confirmed positive cases of COVID-19
Should
Schools should require students and staff to stay home if they are experiencing COVID-19 symptoms or have tested positive for COVID-19.
The guide says schools should require at-home monitoring of symptoms and does not recommend daily symptom screening at school.
If a person is experiencing symptoms at school, schools should ensure the person is wearing a mask and have a designated area where the person is isolated. Symptomatic students should remain under visual adult supervision; that adult should be wearing a mask and maintain 6 feet of distance. School nurses should wear appropriate personal protective gear.
Individuals who are symptomatic or exposed should be given a diagnostic test.
Schools should require students and staff to quarantine if they have been in close contact (within six feet for at least 15 minutes) with a person with a confirmed positive COVID-19 diagnosis, unless:
- The exposed individual is fully vaccinated and does not have symptoms.
- The exposed individual has tested positive for COVID-19 in the past three months, has fully recovered, and does not have symptoms.
- The exposed individual is a student who is not fully vaccinated and both the exposed individual and the infected individual were wearing masks consistently and correctly the entire time.
Schools should work with their local public health department authorities throughout the process — to report positive or presumptive cases, to navigate contact tracing, and to determine the length of the quarantine for infected or exposed individuals.
Go to page 17 for a chart on how long infected and exposed individuals with or without symptoms should quarantine before returning to school. Go here for a CDC chart on interpreting rapid antigen tests.
Could
Schools could consider posting materials about COVID-19 symptoms; educating the school community about symptoms and quarantine policies; offer non-punitive, flexible paid sick leave policies; and develop plans for when employees are on sick leave.
Cleaning and Hygiene
Should
Schools should provide supplies like soap, hand sanitizer, and paper towels for healthy hygiene behaviors and teach adequate hand-washing. That means using soap and water for at least 20 seconds or using a hand sanitizer with at least 60% alcohol for older children and staff.
Schools should clean surfaces once a day. Schools should use an EPA-approved disinfectant for SARS-COV-2 to clean an area in which someone has been sick or tested COVID-19 positive in the last day. Go here for a CDC guide on cleaning and disinfecting your facility.
Could
Schools could encourage people to cough and sneeze into their elbows or into a tissue that is then thrown away, followed by hand-washing. Schools could also set up hand sanitizer at each building entrance and exit, the cafeteria, and in every classroom.
Transportation
Should
Schools should require face coverings during group transportation and keep the windows open if safe and weather permitting. Sick students or drivers should not ride or drive group transportation, and schools should have a plan for how to get sick students home outside of group transportation.
Vehicles should be cleaned regularly and high-touch surfaces should be cleaned before both morning and afternoon routes. Schools should provide hand sanitizer on vehicles.
Could
Schools can consider creating space between students on vehicles when possible and maintaining 3 feet between students and 6 feet between students and the driver.
Water and ventilation systems
Should
Schools should ensure ventilation systems operate properly and consult with heating, ventilation, and air conditioning professionals to consider system improvements. Schools should increase the circulation of outdoor air by opening windows and using fans.
There are a long list of potential strategies and improvements to circulation and central air filtration listed on pages 21 and 22.
Schools should use this CDC guide on ventilation in schools and child care centers and this CDC guide on reopening buildings to ensure water systems and features are safe.
Protecting vulnerable populations
Could
Schools can consider accommodations for students with special health care needs through their individual plans and for teachers who identify as high-risk from COVID-19. Schools can consider creating a process to identify as high-risk and providing alternative student and staff options accordingly, as well as providing remote learning options for students during quarantine or isolation periods.
Additional considerations
Consistent with CDC guidance, the toolkit says health equity is an important aspect to consider in schools’ decision-making and communication with staff and students.
“People living in rural areas, people with disabilities, immigrants, and people who identify as American Indian/Alaska Native, Black or African American, and Hispanic or Latino have been disproportionately affected by COVID-19; these disparities have also emerged among children,” according to the toolkit.
Schools can promote health equity, the guide says, by ensuring students, staff, and families have access to physical and mental health resources and modifying job responsibilities and learning environments based on the needs of individuals. Some modifications may be required by federal law for students with disabilities.
Workers who are older or have certain medical conditions are at higher risk of severe COVID-19 illness, according to the CDC. People with certain underlying conditions or certain medications might still be at risk even if fully vaccinated and might need additional prevention measures. Go here for more.
Recommended reading



