
At the State Health Plan (SHP) Board of Trustees meeting on Tuesday, the board unanimously voted to approve a declaration of intent to implement a tiered-provider structure that would categorize health care providers based on the price of care they negotiate with the SHP. The SHP provides health care coverage to about 750,000 teachers, charter school employees, community college employees, other state employees, retirees, and dependents.
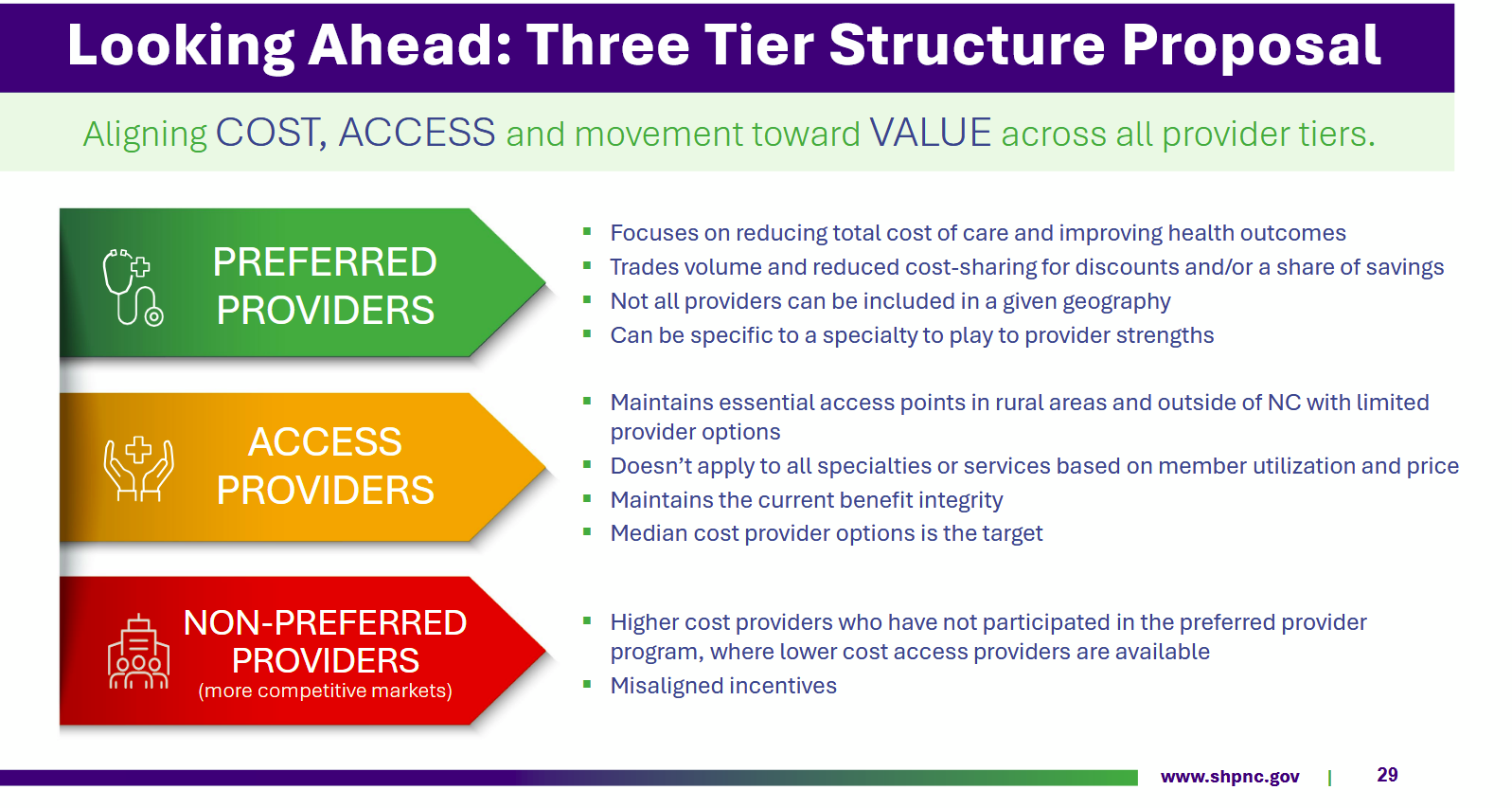
The three tiers of the provider structure would be Preferred, Access, and Non-Preferred, according to meeting materials. SHP members could still use any in-network provider, but the aim is that members would choose preferred providers more often because of their lower out-of-pocket costs.
Those lower costs would be negotiated by the SHP along with potential commitments to better access and quality standards, the board said, in exchange for the increased volume of patients the SHP would steer preferred providers’ way.
![]() Sign up for the EdDaily to start each weekday with the top education news.
Sign up for the EdDaily to start each weekday with the top education news.
The vote comes as State Treasurer Brad Briner, whose office oversees the SHP, is potentially looking to replace Aetna as the plan’s third-party administrator. Aetna replaced Blue Cross and Blue Shield of North Carolina, which administered the SHP for over 40 years, at the beginning of 2025. The switch was voted on in December 2022, under former State Treasurer Dale Folwell.
The plan has faced financial challenges in recent years, at one point facing a $507 million deficit that was projected to grow. Now, following benefit changes and salary-based premium increases, the SHP is “not going to be in a deficit for 2026 or 2027,” said Tom Friedman, executive director of the plan, in December.
However, Friedman said at Tuesday’s meeting, that doesn’t mean the difficulty is over.
“We’re candidly never going to be done having to actively manage this thing,” he said. “It’s not something like you set it and forget it — do two things and be done.”
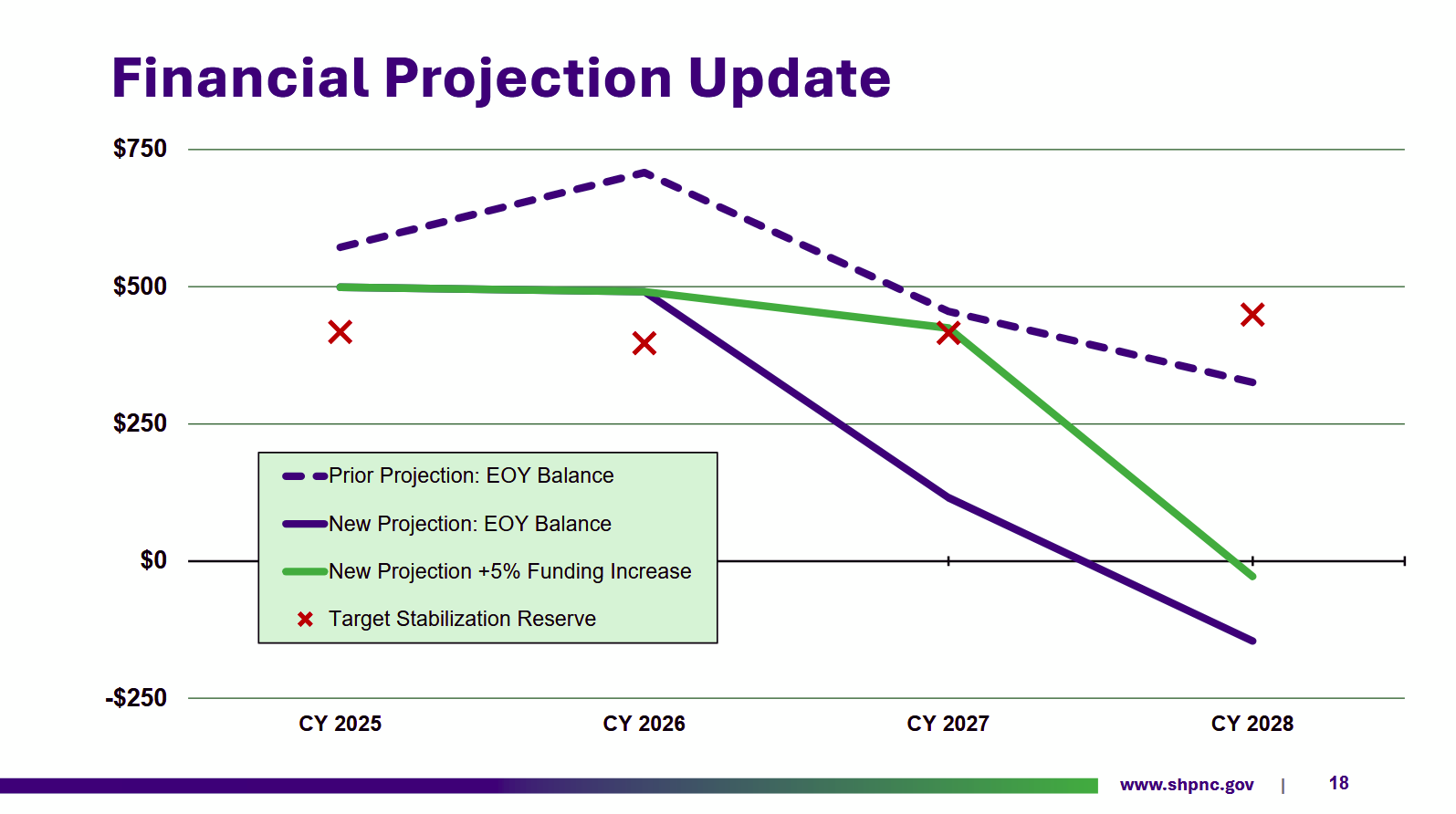
Projections Friedman presented at the meeting showed that, amid rising health care costs, the SHP will stay above its target stabilization reserve level in 2026, and — assuming the General Assembly provides the SHP with a 5% budget increase this year — in 2027.
The plan has asked the General Assembly for a 5% budget increase, according to Dr. Emma Turner, chief economist and director of strategy for the SHP.
Part of ensuring financial stability for the SHP now and past 2027, SHP staff said, is the expansion of cost-saving programs like Lantern Surgical Benefit, which helps members receive surgeries at no cost to them and a lower cost to the SHP.
The shift toward the three-tiered provider structure is another effort to keep the plan’s finances in order and drive down costs for members.
At first, the primary focus areas for negotiating deals to designate preferred providers will be in places where the most services are rendered — usually urban areas with many provider options. According to the presentation, 70% of care to SHP members was rendered in just 10 of North Carolina’s 100 counties.
SHP staff emphasized that the potential savings from moving to the tiered-provider structure are dependent on members seeking preferred providers and potentially changing their care providers when it is cost-effective for them to do so.
“My goal, when this all said and done, is 90% of our members are using a preferred or access provider. I think if we can get there, it is not unrealistic to think we can save $500-$600 million in costs,” Friedman said.
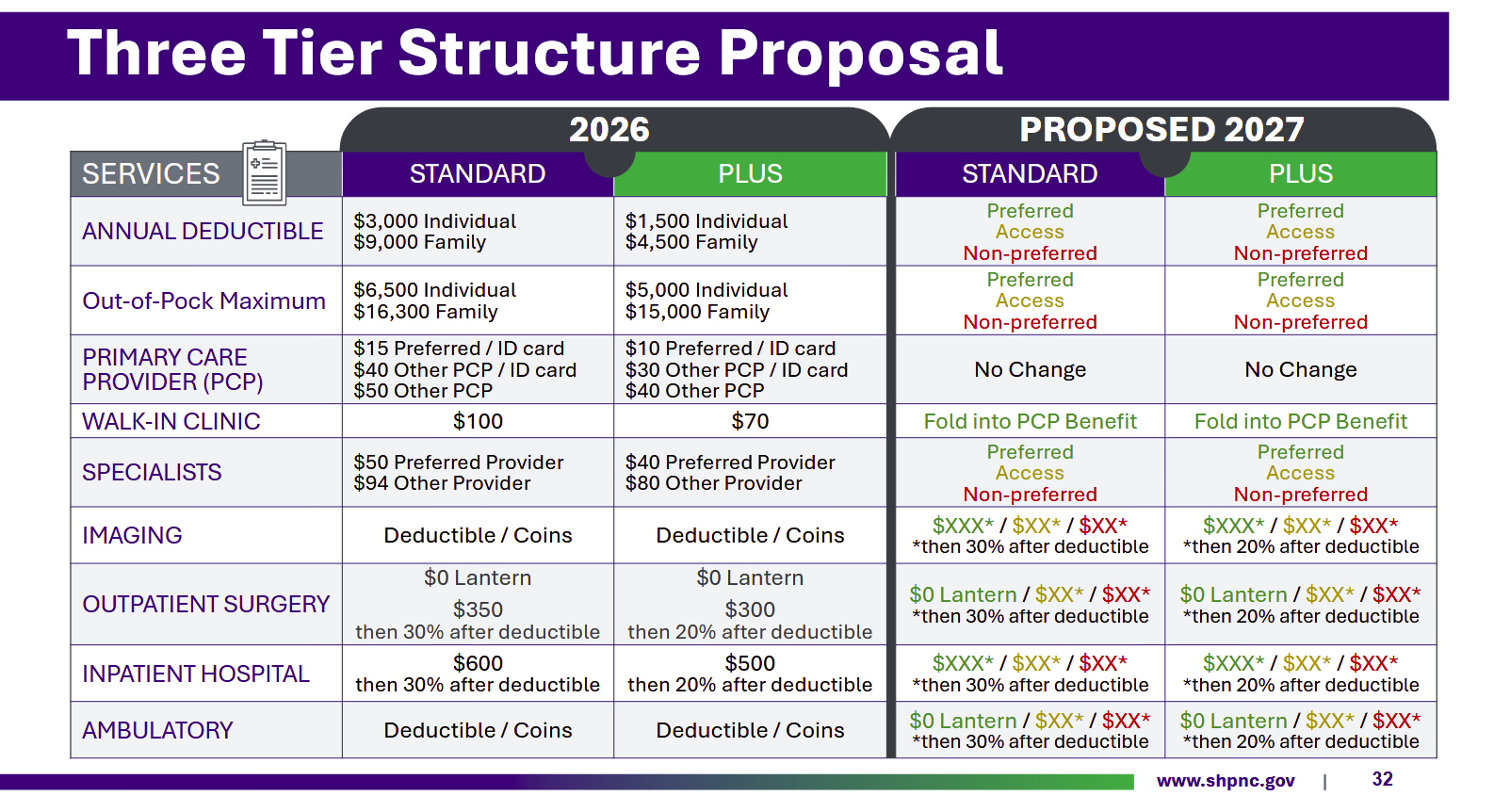
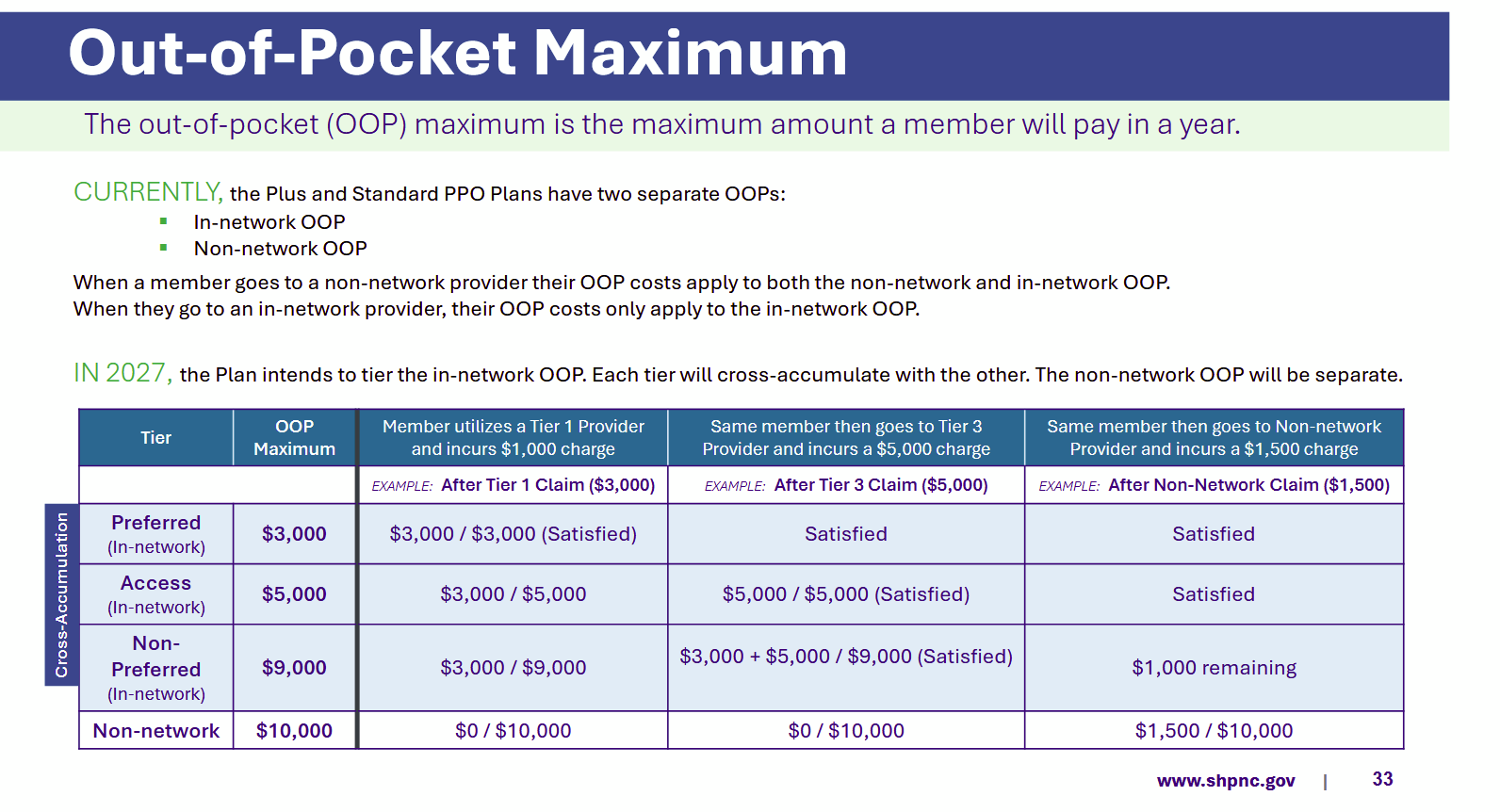
The presentation laid out some potential alternate options to the tiered structure, including across-the-board rate cuts (which providers probably won’t provide), and narrowing the network (which removes choice for members and risks subspecialty access).
But Friedman said the tiered structure is the best option.
“There are alternatives here,” he said. “We just think what we’re proposing is significantly better and more likely to be successful.”
The final copays associated with the tiers are set to be voted on at the SHP’s June 5 meeting, according to a press release from Briner’s office.
Another contributor to financial stability for the SHP is a long-term strategy of proportional salary/premium increases for members, Friedman said. That means that for members, a 1% salary increase would roughly translate to a 1% premium increase.

After the board voted to approve the shift to a tiered-provider structure, Briner thanked board members and staff for their work on navigating tough financial circumstances.
“We are literally rebuilding this plane as we fly it,” Briner said. “We cannot do anything other than keep flying — it’s too important to our members, too important to the entire state.”
Editor’s note: The Blue Cross Blue Shield of North Carolina Foundation supports the work of EdNC.
Recommended reading



